Revolution’s aftermath: population based cross-sectional study to understand the intergeneration mental health and wellbeing following the 2024 student-led uprising
The Child Mind Institute Hosts 2026 Spring Luncheon “Future-Proofing Your Kids: Empowered Parenting in the Digital Age”
New York Times bestselling author Lisa Damour, PhD, led a thoughtful discussion to honor Mental Health Awareness Month
New York, NY – The Child Mind Institute, the leading independent nonprofit dedicated to transforming the lives of children struggling with mental health and learning disorders, hosted its 2026 Spring Luncheon on Monday, May 11. The event featured a dynamic discussion between Lisa Damour, PhD, a three-time New York Times bestselling author and host of the podcast, Ask Lisa: The Psychology of Raising Tweens & Teens, and Dave Anderson, PhD, Vice President of Public Engagement and Education and a senior psychologist at the Child Mind Institute. Their conversation was moderated by Ali Wentworth, an actress, comedian, author, and host of the television show, The Parent Test.
The event brought together advocates and distinguished individuals dedicated to equipping children and families with the skills they need to thrive in today’s rapidly evolving online and social environments. Attendees included Carson and Siri Daly, Jeannie Gaffigan, Kyle MacLachlan, Zibby Owens, and Alysia Reiner.
“We are raising children in a world fundamentally different from any generation before them…a world where childhood unfolds not just in homes and schools but online,” said Harold S. Koplewicz, MD, founding president and medical director of the Child Mind Institute. “Technology brings creativity and connection but also real risks: constant comparison, disrupted sleep, compulsive engagement, and exposure to harmful content. Our job is to help kids build the skills to navigate this world with resilience, confidence, and balance.”
The discussion centered on kids and families and how they can build healthy habits and resilience as they face the demands and distractions of a world increasingly reliant upon and centered around digital technology.
“My umbrella concern is what the conversation about technology is doing to the relationship between adults and kids. The single most powerful force for youth mental health is strong relationships with caring adults,” said Dr. Damour.
“If we focus on driving causal factors — such as family relationships, academic success, in-person friendships, sleep, and movement — we end up promoting a child’s wellness far more than by taking technology away,” said Dr. Anderson.
The luncheon raised over $260,000 to support the Child Mind Institute’s mission to change the lives of children with mental health and learning disorders in the United States and around the world.
The luncheon was co-chaired by Chris Mack, Lisa and Guy Metcalfe, Zibby Owens, and Jil Schaps. The host committee included Robyn and Paul Goldschmid, Desiree Gruber, Molly Jong-Fast, Breanna and John Khoury, Isabelle Krishana, Arielle Tepper, and Sarah J. Wetenhall.
Photos from the luncheon can be found here.
This special event is part of the Child Mind Institute’s programming during Mental Health Awareness Month. The Child Mind Institute recently launched its latest campaign, Mental Health Fitness. Physical fitness doesn’t just happen — it takes skills, regular practice, and a supportive environment. The same is true for mental health. Alongside relatable content from influencers and world-renowned athletes, the Mental Health Fitness resources from the Child Mind Institute provide kids and families with five core mental health skills they can practice every day.
About the Child Mind Institute
The Child Mind Institute is dedicated to transforming the lives of children and families struggling with mental health and learning disorders by giving them the help they need. We’ve become the leading independent nonprofit in children’s mental health by providing gold-standard, evidence-based care, delivering educational resources to millions of families each year, training educators in underserved communities, and developing tomorrow’s breakthrough treatments.
Visit Child Mind Institute on social media: Instagram, Facebook, X, LinkedIn
For press questions, contact our press team at childmindinstitute@ssmandl.com or our media officer at mediaoffice@childmind.org.
The post The Child Mind Institute Hosts 2026 Spring Luncheon “Future-Proofing Your Kids: Empowered Parenting in the Digital Age” appeared first on Child Mind Institute.
Brain Histamine Map Links Genetic Factors to Mental Health and Psychiatric Disorders
A study headed by researchers at King’s College London and the University of Porto has mapped the histamine system in the brain. Histamine, a molecule more commonly associated with allergies, plays a separate but poorly understood role in brain function. The new study addresses this gap, building the first multiscale map of the histamine system which spans from genetics to behavior and related mental health conditions.
The findings provide a new framework for understanding how this often-overlooked chemical system contributes to brain function and could point towards new treatment strategies for histamine-related conditions such as depression, ADHD, and schizophrenia. The study was funded by the National institute for Health and Care Research (NIHR) Maudsley Biomedical Research Centre.
Daniel Martins, MD, PhD, visiting senior research fellow at the Institute of Psychiatry, Psychology & Neuroscience (IoPPN) King’s College London, said, “This work provides a crucial foundation for future research. By integrating molecular biology, brain imaging, and computational analysis, it offers a new perspective on how neurotransmitter systems are organized across the human brain. As neuroscience moves toward more integrated and personalized models of mental health, understanding systems like histamine may prove essential for unlocking new approaches to diagnosis and treatment.”
Martins is first and corresponding author of the team’s published paper in Nature Mental Health, which is titled “Mapping histamine pathway networks in the human brain across cognition and psychiatric disorders.” In their paper the team concluded, “This study provides an integrated characterization of the histaminergic system in the human brain, leveraging transcriptomic, neuroimaging, and functional datasets to delineate its molecular organization and relevance to brain function underlying cognition and psychiatric disorders.”
Histamine is a neurotransmitter, a molecule crucial for neurons to communicate with one another, the authors explained. “Neuronal histamine plays a crucial role in the regulation of brain function, serving as a neuromodulator with widespread influence across multiple neurotransmitter systems.” However, neuroscience research has classically focused on understanding other neurotransmitter systems such as dopamine and serotonin.
As the investigators noted, the organization of histamine in the human brain remains incompletely characterized. However, they explained, dysregulation of the histaminergic system has been implicated in a number of neuropsychiatric conditions, including anxiety, depression, schizophrenia, and autism spectrum disorder (ASD), as well as neurodegenerative diseases including Alzheimer’s, Parkinson’s, and Huntington’s diseases. “Therefore, targeting the brain histamine system has garnered significant attention as a potential new therapeutic strategy for treating these disorders, with pharmacological interventions aimed at modulating histamine receptor activity showing promise in preclinical models.”
Histamine acts through four known histamine receptors, which are responsible for how the signal will influence receiver neurons. Each of these histamine receptors, (histamine receptor H1 (encoded by HRH1), H2 (HRH2), H3 (HRH3) and H4 (HRH4)), mediates distinct functions. For their newly reported study, Martins and colleagues carried out what they described as multimodal analysis, integrating transcriptomic, neuroimaging, developmental and functional datasets to map the architecture of the histaminergic system.
To build a comprehensive map of how histamine acts in the brain, researchers first combined genetic and molecular data with physical maps of the brain.
This revealed which brain regions receive more input from the brain’s histamine system, and which parts show greater capacity to respond to histamine. These molecular data were then linked with positron emission tomography imaging of histamine receptors in living individuals, as well as functional neuroimaging databases that map brain regions to specific cognitive processes and mental health conditions. This type of scan shows how different parts of the brain are working by tracking a tiny amount of radioactive tracer in real time.
Their results found that different histamine receptors were found on brain cells that either turn activity up (excitation) or turn it down (inhibition). “The findings reveal that histaminergic genes exhibit distinct cellular and regional expression profiles, closely aligning with known histaminergic neuroanatomy and function,” they wrote. “At the single-cell level, histamine receptor H1 and histamine receptor H2 were enriched in excitatory neurons, whereas histamine receptor H3 showed preferential expression in inhibitory populations.” This suggests histamine may be important in maintaining the balance between excitation and inhibition, a fundamental property of healthy brain function.
Brain regions with higher histamine-related gene expression were consistently associated with processes such as emotional regulation, stress and fear responses, decision-making, impulsivity, reward, sleep, and memory.
The parts of the brain where histamine-related genes were most active also overlapped significantly with brain regions known to be affected in several psychiatric conditions, including attention-deficit/hyperactivity disorder, major depressive disorder, schizophrenia, and anorexia nervosa. This is in keeping with previous hypotheses linking histamine to these disorders. “By linking histaminergic gene expression to brain-cell types, neurotransmitter systems, cognitive domains and psychiatric disorders, these correlational findings generate several hypotheses concerning histamine’s critical role in brain organization, neurodevelopment and mental health, which further experimental mechanistic work should prioritize and build onto investigate causal relationships,” the investigators concluded.
Martins said, “Current psychiatric treatments largely target neurotransmitters such as serotonin and dopamine, yet histamine interacts closely with these systems and influences their activity. By providing a detailed map of histamine-related pathways, this work suggests new opportunities for developing treatments that target this system more directly, particularly for symptoms such as cognitive dysfunction, fatigue, and impaired motivation.
While these findings do not establish a direct causal role, they suggest that histamine signalling may contribute to regional vulnerability in these disorders. This aligns with a growing view in psychiatry that mental health conditions arise from disruptions across interacting brain systems rather than a single chemical imbalance.”
This new map paints a neural picture of a previously lesser-studied molecule. It opens up future avenues of research into exactly what histamine is doing in various cell types and parts of the brain.
“We want to emphasise that these findings are hypothesis-generating and based on large-scale datasets that capture patterns rather than direct mechanisms,” commented senior author Steve Williams, PhD, professor of neuroimaging at IoPPN King’s College London. Future studies will focus on testing how histamine signaling changes in living individuals, for example through pharmacological interventions or longitudinal imaging approaches.
Co-author Daniel Van Wamelen, PhD, clinical senior lecturer in neuroscience at IoPPN, King’s College London and one of the authors on the paper said: “This kind of work is already taking place at King’s College London, for example in the iMarkHD project. In this project we use Positron Emission Tomography scans to study a specific histamine receptor (called H3) in people with Huntington’s disease, an inherited condition that affects the brain. The goal is to see how histamine activity changes in different parts of the brain over time, and how these changes relate to symptoms such as apathy, depression, and anxiety.”
The post Brain Histamine Map Links Genetic Factors to Mental Health and Psychiatric Disorders appeared first on GEN – Genetic Engineering and Biotechnology News.
Males who discuss suicide seek help less often than females, report finds
Death by suicide is a male emergency. Although three times as many women as men report suicidal ideation and attempts, the vast majority of deaths by suicide in the U.S. — up to 80% — are among men. The reasons: higher impulsivity, lower reported fear of death, and, crucially, easy access to guns.
The most recent report from Crisis Text Line — a nonprofit working with the 988 Suicide & Crisis Lifeline to provide free and confidential text-based mental health support — sheds light on another explanation: Men reach out for help a lot less than women.
Alexa Grasso on Mental Health Fitness
Alexa Grasso shares her routine for staying mentally strong in and out of the Octagon
In recognition of Mental Health Awareness Month, the Child Mind Institute has launched the Mental Health Fitness campaign — a national call to action highlighting the importance that caring for one’s mental health is just as important as physical health.
Alexa Grasso knows the importance of prioritizing her mental well-being alongside her physical training. She uses breathwork to stay grounded, acknowledges emotions instead of suppressing them, and practices mindfulness — highlighting that true strength comes from training the mind with the same discipline as the body.
“What I do when I feel stressed or overwhelmed by life, is breathing. It’s super important to breathe, to think clearly and give time to each emotion. To live it.”
About Anna Sitar
Alexa Grasso is a Mexican mixed martial artist and one of the top competitors in women’s flyweight diving of the UFC. Known for her sharp boxing and calm presence in the Octagon, she made history in 2023 by becoming the first Mexican-born woman to win a UFC championship. Grasso’s rise through the sport has been marked by discipline and resilience, earning her recognition as a trailblazer for Mexican athletes in MMA.
About Mental Health Fitness
For decades, we’ve understood that physical fitness doesn’t just happen — it takes skills, regular practice, and a supportive environment. The same is true for mental health. Developed by experts at the Child Mind Institute for three different age groups, our Mental Health Fitness guides have been used by more than 1.8 million students, caregivers, and educators to build emotion regulation skills and resilience. Whether your child is 5 or 15, struggling or thriving, they can learn these skills. And you can practice alongside them. Learn more at Mental Health Fitness.
Related Resources
- How to Help Children Calm Down
- What Is Co-Regulation?
- How to Model Healthy Coping Skills
- Raising Confident, Independent Children
The post Alexa Grasso on Mental Health Fitness appeared first on Child Mind Institute.
Finding Answers When Your Child Is Struggling: Introducing Ask Kai
Every day, parents reach out to the Child Mind Institute with questions that keep them up at night: Why does my daughter have such strong emotions? Why can’t my son sit still in class? Is this normal anxiety or something more?.
These questions are urgent, but finding answers isn’t easy. The wait time to see a children’s mental health professional can be months or even years. Many families don’t know where to start, what’s normal for their child’s age, or whether their concerns warrant professional help. And with nearly 1 in 5 children experiencing a mental health challenge within the U.S. alone, too many families are navigating this uncertainty on their own.
That’s why we built Ask Kai — a free, evidence-based symptom checker designed specifically for children’s mental health, available in both English and Spanish.
Meet Ask Kai
Ask Kai is a conversational symptom checker that helps parents and caregivers understand their child’s behavior and points them to appropriate resources. Through a streamlined series of questions and prompts, Ask Kai gathers information about your child’s challenges and provides personalized recommendations in minutes.
Ask Kai doesn’t diagnose your child. Instead, it helps you:
- Understand whether your concerns align with common mental health challenges
- Learn what to look for and what questions to ask
- Find evidence-based resources specific to your child’s needs
- Know how to find additional support if needed
Think of Ask Kai as a knowledgeable guide who helps you make sense of what you’re seeing and points you toward your next best step.
How Ask Kai works
If you’ve ever used a symptom checker for physical health, you know the challenge: enter “headache,” and you might walk away convinced you have everything from a sinus infection to a brain tumor. Mental health symptom checkers face even greater challenges. Because every child is different, what looks like defiance in one child could look like anxiety in another, and a behavior that’s appropriate at age five might be cause for concern at age ten. On top of that, mental health conditions often overlap.
So how did we build a tool that captures this complexity without overwhelming families? We focused on expertise and evidence:
- Clinicians and data lead the way: Ask Kai was built using thousands of child mental health evaluations — open datasets spanning different ages, backgrounds, and conditions — and developed in close collaboration with child psychologists and psychiatrists.
- Evidence-based question selection: Rather than asking hundreds of questions, we used machine learning to identify which combinations of questions provide the most meaningful information without burdening families.
- Comprehensive resource library: Every recommendation Ask Kai makes is matched to our extensive collection of guides, articles, expert perspectives, and pathways to professional help.
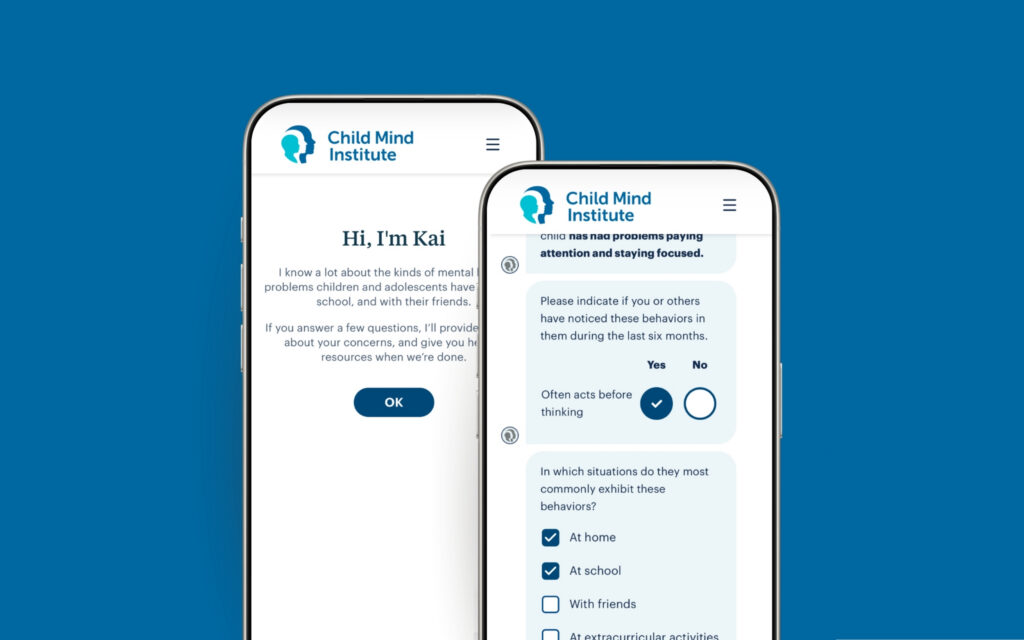
Here’s what happens when you use Ask Kai
Step 1: Initial Screening
You’ll answer a brief set of questions about your child’s behavior, emotions, and how these challenges affect daily life. You’ll also have the chance to describe in your own words what brought you to Ask Kai. These questions cover the areas where we see the most common concerns.
Step 2: Personalized Deep Dive
Based on your responses, Ask Kai selects targeted follow-up questions that dig deeper into the areas you flagged, whether that’s attention and focus, social anxiety, learning, or other behavioral challenges.
Step 3: Matching You to Resources
Ask Kai analyzes your complete response pattern, including the severity and impact of the behaviors you described, and provides a report with recommendations relevant to your child’s age, challenges, and needs.
What Ask Kai can assess
We designed Ask Kai to explore the areas where we can provide the most help to the most families. Ask Kai offers comprehensive screening and resources for:
Attention-deficit/hyperactivity disorder (ADHD) is a neurodevelopmental disorder that is characterized by difficulties with attention, organization, and impulsive behaviors. Symptoms are usually divided into inattentive behaviors or hyperactive and impulsive behaviors. Inattentive symptoms may include making careless mistakes, being easily distracted, difficulty listening to instructions, trouble with organization, and forgetfulness. Hyperactive/impulsive symptoms may include fidgeting or squirming, trouble playing quietly, extreme impatience, as well as constant talking and interrupting.
Autism spectrum disorder (ASD) is a neurodevelopmental disorder that begins in utero, but children may not get diagnosed until they’re in preschool or even older, when symptoms become more apparent. The disorder is characterized by deficits in social communication skills as well as restrictive or repetitive behaviors. Symptoms include a wide range of impaired cognitive abilities, language skills, and behaviors. These symptoms have been thought of as a set of disorders but are now being considered one disorder that presents along a spectrum.
Depression is a mood disorder that can cause children and teenagers to feel very sad and hopeless. Kids with depression have trouble enjoying things they used to love. They may also seem listless and easily annoyed.
Generalized anxiety disorder is characterized by excessive, persistent, and unreasonable worries about everyday things, like doing well in school or sports. In general, kids with this disorder worry a lot about being perfect.
Oppositional defiance disorder is a disruptive behavior disorder characterized by ongoing persistent, age-inappropriate disobedience and resistance to authority. To be diagnosed with this disorder, children would have had to display extreme behavior issues for at least six months. Diagnosis occurs around early elementary school ages and stops around adolescence.
Social anxiety disorder is a type of anxiety characterized by such intense self-consciousness and fear of embarrassment in social situations that the individual avoids social events; also known as social phobia. While some kids with this disorder are specifically afraid of performance engagements like public speaking or sporting events, others are scared of general social situations.
Specific phobia is an anxiety disorder characterized by an excessive and irrational fear of an object, situation, or place. Common specific phobias include dogs, clowns, bugs, the dark, and loud noises.
For young children, bathroom troubles are often a normal part of growing up. But once kids pass potty-training age, peeing or pooping in places other than the toilet might be a sign of an underlying issue. If it involves urine, it’s called “enuresis.” If it involves feces, it’s called “encopresis.”
Nonverbal learning disorder (NVLD) is a condition characterized by difficulty processing visual-spatial information — which involves the brain’s ability to interpret and respond to visual input, including where things are in space. These skills are used to do things like putting together a puzzle or reading a diagram.
Specific learning disorder is a condition that causes children to have difficulty with reading, writing, and/or math. If they have trouble with reading, the disorder is called dyslexia. If they have trouble with writing, it’s called dysgraphia. If they have trouble with math, it’s called dyscalculia. Symptoms are typically first noticed when the child is in preschool or early elementary school.
These ten areas represent some of the most common mental health concerns in childhood. They’re also areas where we have robust data, validated assessments, and comprehensive resources.
What if your concerns aren’t on this list?
Ask Kai can still help. When you describe your situation in your own words, Ask Kai analyzes your response to identify additional concerns and match you to appropriate resources. Your child’s challenges don’t need to fit neatly into one of these categories for Ask Kai to provide value.
However, we will only make recommendations when we’re confident in the evidence behind them. If a particular concern isn’t well represented in our data, we won’t try to provide guidance in that area. Regardless of the results, everyone receives a core set of resources that we believe are helpful for all families navigating children’s mental health.
Your privacy matters
We take data privacy seriously:
- Your responses are confidential and secure
- Free-text responses are analyzed using secure AI systems
- We don’t share your individual information with third parties
- In addition to providing you with resources, your data will only be used to improve Ask Kai
Try Ask Kai Today
If you’re wondering whether your child’s behavior is typical or cause for concern, Ask Kai can help. In just 10 to 15 minutes, you’ll get personalized insights and resources to guide your next steps.
You don’t have to figure this out alone. We’re here to help.
If your child is in crisis, expressing thoughts of self-harm, experiencing severe symptoms, or in immediate danger, please seek emergency help right away. Call 988 (Suicide and Crisis Lifeline), text “HELLO” to 741741 (Crisis Text Line), or go to your nearest emergency room.
Frequently Asked Questions
How long does it take?
Most families complete Ask Kai in 10–15 minutes.
Who should use this tool?
Parents, caregivers, and professionals working with children ages 4–18.
Will I get a diagnosis?
No. Ask Kai provides screening information and resources, but only a qualified clinician can provide a diagnosis.
What if I need immediate help?
If your child is in crisis, please call 988, text “HELLO” to 741741, or visit your nearest emergency room.
What makes this different from other symptom checkers?
Ask Kai was built specifically for children’s mental health, uses evidence-based assessments, provides personalized follow-up questions, and was developed in close collaboration with child mental health professionals.
The post Finding Answers When Your Child Is Struggling: Introducing Ask Kai appeared first on Child Mind Institute.
Enhancing Disability Rights in Europe: Recognition Must Lead to Action
Better recognition, but not enough action: MHE’s initial reaction to the Communication enhancing the Strategy for the Rights of Persons with Disabilities up to 2030 Mental Health Europe (MHE) welcomes […]
The post Enhancing Disability Rights in Europe: Recognition Must Lead to Action appeared first on Mental Health Europe.
Applications Open for the SNF Global Center Communicator Fellowship
The Stavros Niarchos Foundation (SNF) Global Center for Child and Adolescent Mental Health at the Child Mind Institute launches its next two-year fellowship for professionals pursuing evidence-based approaches across diverse, underserved global communities
New York, NY—Applications are now open for the 2026 Communicator Fellowship at the Stavros Niarchos Foundation (SNF) Global Center for Child and Adolescent Mental Health at the Child Mind Institute. The fellowship is designed to support a new generation of communicators working to shape child and adolescent mental health care in low- and middle-income countries, in addition to the SNF Global Center’s core country offices in Brazil, Greece, and South Africa. Up to three professionals working in public communications, including journalists, broadcasters, and podcasters, will be selected for the two-year program.
The Communicator Fellowship is part of the SNF Global Center’s broader mission to reduce gaps in data and care, catalyze system-level advancements, and transform child and adolescent mental health care by turning evidence into action, scaling culturally appropriate solutions, and building a global network of experts so young people everywhere can access support when they need it.
The application deadline is June 15, 2026. Fellows will be selected and announced by early August 2026. In addition to financial support of up to $100,000 USD, fellows will receive training, mentorship, and networking opportunities.
At a time when one in five young people are experiencing mental health or learning challenges, with most cases beginning by age 14, effective and accurate communication is urgently needed.
At the Child Mind Institute, we believe that translating research into accessible knowledge that empowers young people, families, and communities is integral to advancing mental health care. The Communicator Fellowship builds on this commitment by supporting professionals who can bring evidence-based mental health information to the public in clear, engaging, and culturally relevant ways.
Vinicius Gaby Vieira Rego, MD, of Brazil, a current Communicator Fellow with the support of the Institute of Psychiatry at the University of São Paulo, exemplifies this mission. Working with youth, Dr. Rego is co-creating a multi-platform literacy hub designed to combat harmful misinformation by empowering Brazil’s young leaders.
“I am deeply grateful for the opportunity to join the SNF Global Center’s network of fellows to support adolescent mental health in Brazil through communication,” said Dr. Rego. “This fellowship will enable a multi-channel communication project aimed at strengthening mental health literacy and peer-support capacity — with young people and for young people — across the country.”
As a fellow, Dr. Rego’s work directly addresses complex mental health challenges faced by young people in Brazil, while contributing to broader global efforts to improve communication about mental health care.
“In the current digital environment, where adolescents are exposed to a high volume of mental health content, the need for evidence-based information that resonates with young people has never been greater,” said Guilherme Polanczyk, MD, PhD, associate professor of Child and Adolescent Psychiatry at the University of São Paulo. “We are proud to endorse a project committed to supporting how young people and their communities understand and reflect on their mental health.”
Other current fellows are leading high-impact projects dispelling misinformation, reducing stigma, and increasing youth engagement — all while bringing critical attention to links among mental health, climate change, and human rights. Through partnerships, these efforts are transforming the future of youth mental health across the globe.
“Vinicius’s project is ambitious, and with the support of the Institute of Psychiatry at the University of São Paulo, we know it will provide young people in Brazil with much-needed resources to support their mental health,” said Peter Raucci, Director of Global Fellowship Strategy of the SNF Global Center at the Child Mind Institute. “What we’re seeing through the Communicator Fellowship is how quickly ideas can move from concept to culturally relevant, real-world impact.”
SNF Global Center Communicator Fellowship
Application deadline: June 15, 2026
Fellows announced: August 2026
Program resources
About the SNF Global Center at the Child Mind Institute
The Stavros Niarchos Foundation (SNF) Global Center for Child and Adolescent Mental Health at the Child Mind Institute brings together the Child Mind Institute’s expertise as a leading independent nonprofit in children’s mental health and the Stavros Niarchos Foundation’s deep commitment to supporting collaborative projects to improve access to quality health care worldwide. The center is building partnerships to drive advances in under-researched areas of children and adolescents’ mental health, and expand access to culturally appropriate training, resources, and treatment in low- and middle-income countries. This work is conducted by the Child Mind Institute with support from SNF through its Global Health Initiative (GHI).
About the Child Mind Institute
The Child Mind Institute is dedicated to transforming the lives of children and families struggling with mental health and learning disorders by giving them the help they need. We’ve become the leading independent nonprofit in children’s mental health by providing gold-standard, evidence-based care, delivering educational resources to millions of families each year, training educators in underserved communities, and developing tomorrow’s breakthrough treatments.
The post Applications Open for the SNF Global Center Communicator Fellowship appeared first on Child Mind Institute.

