Finding Answers When Your Child Is Struggling: Introducing Ask Kai
Every day, parents reach out to the Child Mind Institute with questions that keep them up at night: Why does my daughter have such strong emotions? Why can’t my son sit still in class? Is this normal anxiety or something more?.
These questions are urgent, but finding answers isn’t easy. The wait time to see a children’s mental health professional can be months or even years. Many families don’t know where to start, what’s normal for their child’s age, or whether their concerns warrant professional help. And with nearly 1 in 5 children experiencing a mental health challenge within the U.S. alone, too many families are navigating this uncertainty on their own.
That’s why we built Ask Kai — a free, evidence-based symptom checker designed specifically for children’s mental health, available in both English and Spanish.
Meet Ask Kai
Ask Kai is a conversational symptom checker that helps parents and caregivers understand their child’s behavior and points them to appropriate resources. Through a streamlined series of questions and prompts, Ask Kai gathers information about your child’s challenges and provides personalized recommendations in minutes.
Ask Kai doesn’t diagnose your child. Instead, it helps you:
- Understand whether your concerns align with common mental health challenges
- Learn what to look for and what questions to ask
- Find evidence-based resources specific to your child’s needs
- Know how to find additional support if needed
Think of Ask Kai as a knowledgeable guide who helps you make sense of what you’re seeing and points you toward your next best step.
How Ask Kai works
If you’ve ever used a symptom checker for physical health, you know the challenge: enter “headache,” and you might walk away convinced you have everything from a sinus infection to a brain tumor. Mental health symptom checkers face even greater challenges. Because every child is different, what looks like defiance in one child could look like anxiety in another, and a behavior that’s appropriate at age five might be cause for concern at age ten. On top of that, mental health conditions often overlap.
So how did we build a tool that captures this complexity without overwhelming families? We focused on expertise and evidence:
- Clinicians and data lead the way: Ask Kai was built using thousands of child mental health evaluations — open datasets spanning different ages, backgrounds, and conditions — and developed in close collaboration with child psychologists and psychiatrists.
- Evidence-based question selection: Rather than asking hundreds of questions, we used machine learning to identify which combinations of questions provide the most meaningful information without burdening families.
- Comprehensive resource library: Every recommendation Ask Kai makes is matched to our extensive collection of guides, articles, expert perspectives, and pathways to professional help.
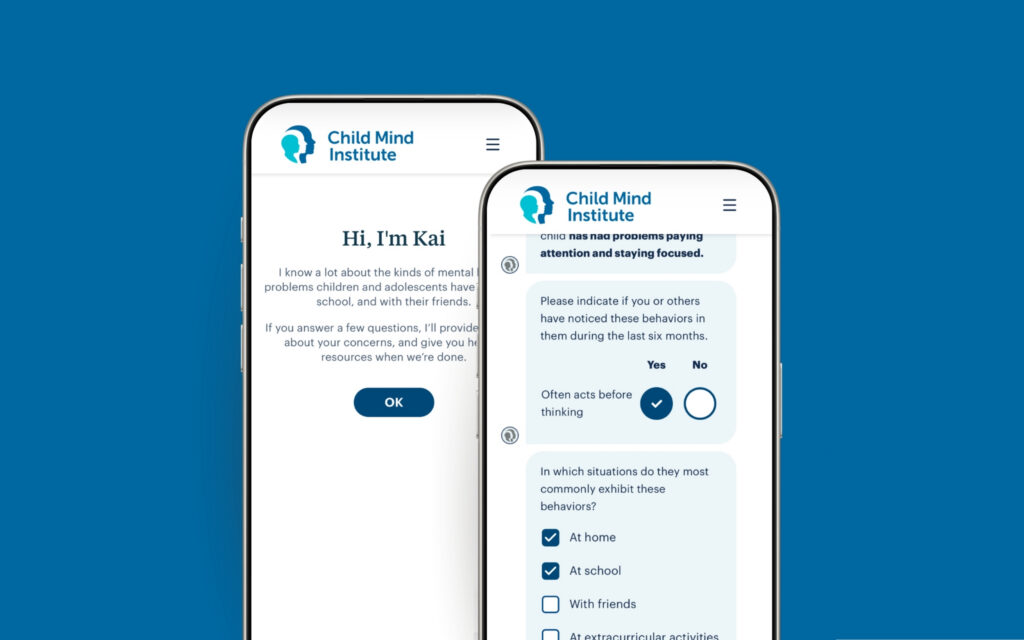
Here’s what happens when you use Ask Kai
Step 1: Initial Screening
You’ll answer a brief set of questions about your child’s behavior, emotions, and how these challenges affect daily life. You’ll also have the chance to describe in your own words what brought you to Ask Kai. These questions cover the areas where we see the most common concerns.
Step 2: Personalized Deep Dive
Based on your responses, Ask Kai selects targeted follow-up questions that dig deeper into the areas you flagged, whether that’s attention and focus, social anxiety, learning, or other behavioral challenges.
Step 3: Matching You to Resources
Ask Kai analyzes your complete response pattern, including the severity and impact of the behaviors you described, and provides a report with recommendations relevant to your child’s age, challenges, and needs.
What Ask Kai can assess
We designed Ask Kai to explore the areas where we can provide the most help to the most families. Ask Kai offers comprehensive screening and resources for:
Attention-deficit/hyperactivity disorder (ADHD) is a neurodevelopmental disorder that is characterized by difficulties with attention, organization, and impulsive behaviors. Symptoms are usually divided into inattentive behaviors or hyperactive and impulsive behaviors. Inattentive symptoms may include making careless mistakes, being easily distracted, difficulty listening to instructions, trouble with organization, and forgetfulness. Hyperactive/impulsive symptoms may include fidgeting or squirming, trouble playing quietly, extreme impatience, as well as constant talking and interrupting.
Autism spectrum disorder (ASD) is a neurodevelopmental disorder that begins in utero, but children may not get diagnosed until they’re in preschool or even older, when symptoms become more apparent. The disorder is characterized by deficits in social communication skills as well as restrictive or repetitive behaviors. Symptoms include a wide range of impaired cognitive abilities, language skills, and behaviors. These symptoms have been thought of as a set of disorders but are now being considered one disorder that presents along a spectrum.
Depression is a mood disorder that can cause children and teenagers to feel very sad and hopeless. Kids with depression have trouble enjoying things they used to love. They may also seem listless and easily annoyed.
Generalized anxiety disorder is characterized by excessive, persistent, and unreasonable worries about everyday things, like doing well in school or sports. In general, kids with this disorder worry a lot about being perfect.
Oppositional defiance disorder is a disruptive behavior disorder characterized by ongoing persistent, age-inappropriate disobedience and resistance to authority. To be diagnosed with this disorder, children would have had to display extreme behavior issues for at least six months. Diagnosis occurs around early elementary school ages and stops around adolescence.
Social anxiety disorder is a type of anxiety characterized by such intense self-consciousness and fear of embarrassment in social situations that the individual avoids social events; also known as social phobia. While some kids with this disorder are specifically afraid of performance engagements like public speaking or sporting events, others are scared of general social situations.
Specific phobia is an anxiety disorder characterized by an excessive and irrational fear of an object, situation, or place. Common specific phobias include dogs, clowns, bugs, the dark, and loud noises.
For young children, bathroom troubles are often a normal part of growing up. But once kids pass potty-training age, peeing or pooping in places other than the toilet might be a sign of an underlying issue. If it involves urine, it’s called “enuresis.” If it involves feces, it’s called “encopresis.”
Nonverbal learning disorder (NVLD) is a condition characterized by difficulty processing visual-spatial information — which involves the brain’s ability to interpret and respond to visual input, including where things are in space. These skills are used to do things like putting together a puzzle or reading a diagram.
Specific learning disorder is a condition that causes children to have difficulty with reading, writing, and/or math. If they have trouble with reading, the disorder is called dyslexia. If they have trouble with writing, it’s called dysgraphia. If they have trouble with math, it’s called dyscalculia. Symptoms are typically first noticed when the child is in preschool or early elementary school.
These ten areas represent some of the most common mental health concerns in childhood. They’re also areas where we have robust data, validated assessments, and comprehensive resources.
What if your concerns aren’t on this list?
Ask Kai can still help. When you describe your situation in your own words, Ask Kai analyzes your response to identify additional concerns and match you to appropriate resources. Your child’s challenges don’t need to fit neatly into one of these categories for Ask Kai to provide value.
However, we will only make recommendations when we’re confident in the evidence behind them. If a particular concern isn’t well represented in our data, we won’t try to provide guidance in that area. Regardless of the results, everyone receives a core set of resources that we believe are helpful for all families navigating children’s mental health.
Your privacy matters
We take data privacy seriously:
- Your responses are confidential and secure
- Free-text responses are analyzed using secure AI systems
- We don’t share your individual information with third parties
- In addition to providing you with resources, your data will only be used to improve Ask Kai
Try Ask Kai Today
If you’re wondering whether your child’s behavior is typical or cause for concern, Ask Kai can help. In just 10 to 15 minutes, you’ll get personalized insights and resources to guide your next steps.
You don’t have to figure this out alone. We’re here to help.
If your child is in crisis, expressing thoughts of self-harm, experiencing severe symptoms, or in immediate danger, please seek emergency help right away. Call 988 (Suicide and Crisis Lifeline), text “HELLO” to 741741 (Crisis Text Line), or go to your nearest emergency room.
Frequently Asked Questions
How long does it take?
Most families complete Ask Kai in 10–15 minutes.
Who should use this tool?
Parents, caregivers, and professionals working with children ages 4–18.
Will I get a diagnosis?
No. Ask Kai provides screening information and resources, but only a qualified clinician can provide a diagnosis.
What if I need immediate help?
If your child is in crisis, please call 988, text “HELLO” to 741741, or visit your nearest emergency room.
What makes this different from other symptom checkers?
Ask Kai was built specifically for children’s mental health, uses evidence-based assessments, provides personalized follow-up questions, and was developed in close collaboration with child mental health professionals.
The post Finding Answers When Your Child Is Struggling: Introducing Ask Kai appeared first on Child Mind Institute.
The dual-burden of professional and academic stress: a cross-sectional mapping of mental health status and coping efficacy among postgraduate students in Nairobi, Kenya
Surf Therapy: A Powerful Low-Intensity Approach in Global Youth Mental Health Care
By Mai El Shoush, Partnerships Campaign Manager, Stavros Niarchos Foundation (SNF) Global Center for Child and Adolescent Mental Health at the Child Mind Institute
In Conversation with Waves for Change
The world’s oceans have long been profound forces that shape coastlines, cultures, and scientific discovery. And today, through targeted programs, they also serve as therapeutic environments transforming youth mental health worldwide.
As global health systems continue to explore solutions that minimize resource constraints while addressing child and adolescent mental health demands, innovative approaches like surf therapy are demonstrating remarkable effectiveness as low-intensity initiatives. From the beaches of California to the coastal communities of South Africa, Australia, Hawai’i, the United Kingdom, and Senegal, these programs are creating accessible entry points for young people.
Wave for Change (W4C) — a South Africa-based organization and valued implementation partner of the Stavros Niarchos Foundation (SNF) Global Center at the Child Mind Institute — has developed an evidence-based Surf Therapy program for youth in underserved communities. We spoke with their chief development officer Paula Yarrow and senior grant manager Jill Sloan about the award-winning program. As a highly regarded Cape Town‑based NGO that uses surfing as a therapeutic tool to support youth mental health, W4C offers safe spaces, evidence‑based emotional regulation tools, community mentorship, and a pathway to resilience for young people growing up in challenging environments.
The partnership includes the identification of workforce gaps and training needs for frontline workers such as NGOs, to further expand evidence-based support and brief interventions through culturally appropriate, low-intensity psychological therapy approaches. The context-specific training materials are expected to be piloted later in the year in South Africa and are intended to improve access to quality mental health care for young people.
W4C launched Surf Therapy in 2009, which has since helped more than 10,000 adolescents experiencing high-stress environments gain valuable coping skills across its hubs in the Western and Eastern Cape as well as Cape Town. Participants learn how to build positive social networks and develop self-regulation skills to support healthy emotional and behavioral responses to stress, with coaches themselves aged between 18-25. The program creates a fun, culturally relevant environment through the Take 5 model — a framework W4C has designed to be adapted for a range of sports, arts, and cultural initiatives. The model has been utilized by several leading global organizations, including UNICEF.
Waves for Change also played a key role in the founding of the International Surf Therapy Organization (ISTO), connecting practitioners, clinicians, and researchers to advance science research, raise awareness, and support surf therapy.

How does Waves for Change use evidence-based Surf Therapy and capacity building as a solution to fill the gap in youth mental health care?
Approximately 90 percent of the world’s adolescents live in low- and middle-income countries (LMICs). In the most underserved communities, adolescents may experience repeated exposure to violence, unmet basic needs, and limited access to safe spaces or trusted caregivers. Typically, there are very few mental health services that are accessible to such youth.
The more Adverse Childhood Experiences (ACEs) a child or adolescent has whilst growing up, the more likely they are to develop toxic stress — an ongoing stress state without respite. This can often lead to mental health conditions such as anxiety, depression, substance misuse, and cognitive impairment. This can also result in the development of physical health conditions such as heart disease as they grow into adulthood.
The main problem we’ve identified is that there aren’t enough trained workforces (e.g., sports coaches, youth facilitators) that are able to deliver simple, fun, structured play-based sessions with consistency at scale. Our work provides a response to this issue within the adolescent mental health promotion and illness prevention arena. Additionally, our initiatives significantly increase the number of individuals — coaches, teachers, mentors or others — who are already in contact with young adolescents and can provide them with mental health support to foster their immediate and longer-term mental health.
How has Waves for Change adapted the organization’s Surf Therapy program to develop the Take 5 model?
Waves for Change’s Take 5 training model has been incubated, tested, and rigorously evaluated within W4C’s award-winning Surf Therapy program. Take 5 distils the key components of our Surf Therapy program, providing coaches with the essential skills they need to build and sustain caring relationships with children. And it uses a simple teaching routine that creates consistently engaging, fun, structured programs for children and adolescents that suit their language, culture, and context.
Take 5 is low intensity and cost-effective — tailored for high-stress environments and the unique mental wellness needs of adolescents living in multidimensional poverty, conflict, or crisis.
How has partnering with young people to research and co-develop programs made the work more impactful?
In research studies we’ve conducted, adolescent participants (ages 10-16) reported experiencing between 6-8 adverse events every year, including violence and abuse. When asked what sorts of spaces they wanted to see at Waves for Change, the adolescents identified core components such as access to a safe space where they could have fun, be heard, and learn skills to cope. These components now form the bedrock of our Surf Therapy program. We initially worked with 9-12-year-olds and have since developed the follow-on programme for adolescents up to age 16 who have graduated the Surf Therapy programme. This is called Surf Club and is available to all Surf Therapy graduates.
Waves for Change also conducts pre- and post-intervention surveys with participants to monitor the impact of our work. Our coaches (ages 18-25) are at the frontline of delivering our services. A key role they play is to listen with care and respect to the adolescents’ concerns, and to share them with our Child Protection team for review and follow-up when needed.

What makes your partnership with the SNF Global Center at the Child Mind Institute unique?
Working with the Child Mind Institute allows Waves for Change to collaborate with and learn from colleagues doing similar work in the adolescent mental health space across South Africa, the United Kingdom, and Brazil. The partnership offers an opportunity to learn about approaches that have been successful in other health systems. It has also allowed Waves for Change to share detailed information about the training and supervision protocol used to develop key competencies in the coach workforce that leads Surf Therapy in South Africa. This has helped the Child Mind Institute to develop a comprehensive guide for other similar workforces.
Can you expand on the importance of partnerships in strengthening youth mental health care and community empowerment?
Partnerships allow for the consolidation of skills and resources so that a greater impact can be achieved. For example, at Waves for Change, we work with over 70 referral partners every year to identify young adolescents who can benefit from our Surf Therapy program. We are also partnering with the Department of Cultural Affairs and Sport to use our Take 5 model to train MOD and YearBeyond coaches and mentors, who are already reaching large numbers of children and young adolescents through their work. And we’re contributing to building the broader ecosystem of mental health support for adolescents and children by training large national NGOs, government agencies, and humanitarian organizations with our Take 5 model.
How can non-profits further help foster strong peer networks and inclusive safe spaces?
Some of the key lessons we have learnt are the following:
- In the field of youth mental health, make youth the leaders on program implementation
- Provide youth with skills, opportunities, supervision, and support so that they can grow and develop further
- Maintain a strong culture of protection, respect, and communication so that all participants feel safe, welcome, accepted, and heard
Read more about W4C’s Surf Therapy from Youth Liaison Officer, Azola Sibanda and Training Manager Jamie-Lee Davids
The post Surf Therapy: A Powerful Low-Intensity Approach in Global Youth Mental Health Care appeared first on Child Mind Institute.
Exercise as a multiscale recalibration of stress-related homeostatic balance
The correlation between phubbing and depression anxiety stress of first-year medical students: the mediating role of sedentary behavior
Autonomic nervous system reactions to secondary exposure to disaster-related imagery
Joint latent profiles of death anxiety and treatment adherence in HCC patients
Calming Minds Study
Interventions: Behavioral: Be Specific; Behavioral: Be Kind; Behavioral: Be Present; Behavioral: Break Habit; Behavioral: Psychoeducation
Sponsors: University of California, Los Angeles; University of Exeter
Not yet recruiting
Comorbidity alters the genetic relationship between anxiety disorders and major depression
The extensive genetic overlap between anxiety disorders (ANX) and major depression (MD) may partly reflect inclusion of comorbid cases in genome-wide association studies (GWAS). We investigated this genetic relationship between ANX and MD with and without mutual comorbidity.

